Resources for Clinicians
Welcome to the Identification, Assessment and Diagnosis Hub for Prenatal Alcohol Exposure and FASD (IAD Hub). The IAD Hub was developed to support health and allied health care providers across all settings—primary care, specialty care, public health, mental health, and beyond—with the most current tools and resources to improve early identification, diagnostic decision-making, and referral coordination. Whether you are starting a conversation about alcohol use in pregnancy or navigating a complex referral, the IAD hub is your one-stop access point to evidence-based, Canadian-specific FASD resources.
Identification and Early Intervention
Fetal Alcohol Spectrum Disorder (FASD) is a common lifelong disability, but it often goes under-recognized and under-diagnosed. Identification of possible FASD involves identifying people who have prenatal alcohol exposure (PAE) and are exhibiting behaviours that may be associated with FASD. Professionals can then refer them to the appropriate FASD diagnostic services.
Identification of possible FASD is the only the first step: ensuring there are FASD-informed services and interventions available to support the individual and their diagnosis is essential.
Established prenatal alcohol exposure (PAE) is often a requirement for referral to a specialized diagnostic clinic. There is currently not a standardized, validated identification tool for FASD, although the diagnostic criteria (facial features, significant brain domain impairment and prenatal alcohol exposure) are well-established. Clinicians rely on informal intake conversations, clinical observation, or the use of tools designed for other conditions (e.g., Attention Deficit Hyperactivity Disorder, anxiety, trauma, adverse childhood experiences) as well as possible or confirmed prenatal alcohol exposure. Clinics may be able to access PAE information from friends or family or from birth, medical and/or social services records.
“The most effective tool is [to] have the time to listen … just sit and listen. … For too many, this is the first time their story has been shared with anyone.”
Discussing Alcohol Use
Confirming and documenting prenatal alcohol exposure (PAE) is challenging, and represents a major barrier to accurate identification and diagnosis of FASD.
Conversations are often emotionally complex, ethically fraught, and deeply influenced by stigma, trauma, and fear of blame. Like identification of FASD, PAE information is collected in a variety of ways, ranging from informal conversations and collateral reports to the use of locally developed questionnaires or checklists.
Guideline No. 405: Screening and Counselling for Alcohol Consumption During Pregnancy from the Society of Obstetricians and Gynaecologists of Canada recommends that all pregnant women are screened for alcohol use.
Alcohol Screening Tools
ASSIST: The Alcohol, Smoking and Substance Involvement Screening Test. (English). A 8-item questionnaire used to screen for substance use across a variety of substances.·
T-ACE: Tolerance, Annoyed, Cut Down, Eye-Opener. (English). A 4-item questionnaire to determine at-risk drinking.
TWEAK: Tolerance, Worry, Eye-opener, Amnesia, K/Cut down. (English). A 5-item, 7 point questionnaire used to assess at-risk drinking.
AUDIT-C: brief alcohol consumption screener. (English). A 3-item, 12 point self-report questionnaire used to assess at-risk drinking.
Collecting Information About Prenatal Alcohol Exposure
The Lakeland Centre for FASD, Rajani Clinic Training Services recently developed a new toolkit to support FASD Diagnostic Clinics in collecting information about PAE.
- New Resource: A Toolkit to Support PAE Collection in FASD Diagnostic Clinics. (English | French). Available on request from Rajani Clinic Training Services. An evidence-based screening and identification tool made to establish consistent practices and share practical strategies for navigating the conversation and verification of client history.
Navigating Conversations about Alcohol Use During Pregnancy
Current resources and advice emphasize the importance of experience in navigating conversations about alcohol and pregnancy, which can be sensitive and complex. Mentors with more experience can be helpful for those with less experience. Having frequent conversations with all families is a good way to reduce the stigma associated with alcohol use during pregnancy and normalize the conversation.
Alcohol in pregnancy is everyone’s business
Asking questions about alcohol in pregnancy
Recording alcohol use in pregnancy
Conversations about alcohol and pregnancy should be in plain language, where information is presented in multiple ways (e.g., graphs, diagrams, videos, statistics). Offer a choice to the individuals/families about how they would like to receive education and information, and with whom—including in-person and virtual options depending on personal preference and comfort.
Tips for having conversations about alcohol use in pregnancy:
Prioritize feelings of safety.
- Ensure safety through the physical environment of the clinic (i.e. flexibility in sensory accommodation), cultural considerations, and client choice on how and when to receive information.
Be direct, but compassionate.
- Honesty and directness stem from a non-judgemental, compassionate approach; working from a lens to plan for a path forward, as opposed to focusing on problems and/or the past.
- Determine the clients’ knowledge level of FASD at the start of any conversation; be aware that everyone has a story, and that that story may come with potential trauma.
Focus on listening and respect.
- Conversations around FASD require connection: taking the time to form meaningful relationships, listening, normalizing difficult situations in life, affirming the decision to seek a diagnosis, treating alcohol use like other general nutrition information/other medical history, and focusing on interventions, therapies and supports that strengthen skills, while also identifying supports for limitations.
- Remember that the goal is to find ways to support the individual, family, school and community.
Tools and Resources on Identification of FASD
- New Resource: A Toolkit to Support PAE Collection in FASD Diagnostic Clinics. (English | French). Available on request from Rajani Clinic Training Services. An evidence-based screening and identification tool made to establish consistent practices and share practical strategies for navigating the conversation and verification of client history.
- Talking with children, adolescents and adults about FASD / Other Brain-Based Conditions. (English.) A resource for introducing the topic of FASD to families and individuals.
- FASCETS Exploration Tool. (English.) A tool to explore client neurodiversity. Please note that tool access is locked behind completion of training.
- Two-Eyed Seeing Tools for Screening, Assessment, Intervention and Prevention. (English.) Inspired by Mi’kmaq Elders, Two-Eyed Seeing (TES) tools integrate a traditional healing perspective into the medical assessment process. This includes the Medicine Wheel Developmental History tool—a semi-structured interview tool that aims to allow mothers to tell their story.
- Neurobehavioural Screening Tool. (English.) A brief screening tool where primary and secondary characteristics are rated on a scale of 0-5. Not specific to FASD.
Resources on Conversations and Support about PAE
- Asking About Prenatal Substance Exposure in Pediatric Populations: A toolkit for clinicians working with children and families. (English). (2024). A toolkit on asking about PAE, including quick guides on when to ask, how to ask, and why it matters.
- The Prevention Conversation. (English). An online training program to support frontline service providers in leading supportive, non-judgemental discussions about alcohol use during pregnancy.
- Identifying Best Practices for FASD. (English | French). An online training course that includes resources on how to identify and screen for individuals with FASD and strategies to support individuals in achieving healthy outcomes.
- A Digital Handbook on Wraparound Programs. (English | French). (2023). A digital handbook made to support the creation and sustainment of wraparound programs for pregnant and/or early parenting people with substance use and other concerns.
Identification of and discussions around alcohol use, pregnancy and FASD do not exist in isolation. Conversations may also be had about prevention, breastfeeding, and other related topics. For more information, see Prevention – CanFASD.
Referral Pathways
Effective referral ensures timely diagnosis and appropriate supports and services for individuals affected with Fetal Alcohol Spectrum Disorder (FASD). However, referral pathways are fragmented across Canada. Different clinics have different eligibility criteria, documentation requirements, and wait times. Families and individuals may struggle to understand where to go, what to expect, and how long the process will take; in many cases, support in navigating these systems may fall to clinicians.
This webpage was designed to support health, allied health and social service providers to navigate effective referrals for FASD diagnosis.
Referral Pathways.
The first step in referral for an FASD diagnosis is understanding the eligibility criteria/requirements for the clinic or pathway which may include:
- Region (e.g., clinics may only accept referrals from their local community)
- Age (e.g., clinics may be child or adult only)
- Individual who is referring (e.g., clinics may accept self-referral, rely on service providers, or have their own referral process)
- Service or programming (e.g., some referrals require involvement in a relevant program that may help prepare for assessment and promote coordinated, wraparound approaches)
Clinics may use referral forms that are publicly available, or may need to be contacted directly by phone or email. Referral pathways differ depending on clinic, network and area of Canada, but history and information are important first steps in the assessment process.
Community Support FASD Networks and Resources.
Please note that this list is not comprehensive, as many smaller regions and communities have their own organizations.
- Manitoba: Manitoba FASD Network
- Ontario: FASD ONE and FASD / TSAF – Ontario
- Newfoundland and Labrador: fasd NL
- PEI: The fasd NL – Atlantic Community Network Blog also brings together people from the Atlantic provinces (Nova Scotia, New Brunswick, Prince Edward Island, Newfoundland and Labrador).
- Nova Scotia: Fetal Alcohol Nova Scotia (FANS)
- New Brunswick: NB FASD Centre of Excellence – Vitalité | Francophone leader serving its communities
- Saskatchewan: FASD Network of Saskatchewan
- Alberta: FASD Alberta
- British Columbia: FASD Society For BC – The Asante Centre PLEA Community Services
- Northwest Territories: Fetal Alcohol Spectrum Disorder | Foster Family Coalition
- The Yukon: FASSY
- Nunavut: Piruqatigiit Resource Centre
CanFASD has also compiled a list of local caregiver and community agencies/supports.
For more resources for individuals with FASD and their families, please see the Identification, Assessment and Diagnosis Hub for Individuals with FASD, Caregivers and Advocates.
Diagnosis and Clinical Guidance
Diagnosing Fetal Alcohol Spectrum Disorder (FASD) is a critical step in ensuring individuals receive the care, support, and understanding they need to thrive. The diagnostic process involves a comprehensive assessment of neurodevelopmental functioning, physical features, and prenatal alcohol exposure (PAE) history, guided by nationally recognized criteria. This section provides health care providers with the tools and resources to navigate the complexities of FASD diagnosis across age groups from infancy to adulthood.
The purpose of this page is to provide evidence-based guidance and practical tools to support the accurate and timely diagnosis of FASD.
Resources:
- Guidelines for Assessing and Diagnosing FASD (English | French). Published in 2016, Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan (English | French) provides evidence-based diagnostic criteria to assist multidisciplinary teams through the diagnostic process. Executive Summary | Appendix 1
- Multidisciplinary Team Training for Diagnosis of FASD (English | French). This online FASD curriculum, based on Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan (English | French). has been developed to assist professionals in learning the processes and procedures, and in developing the skill set needed to be effective members of a multidisciplinary diagnostic team.
- Trouble du spectre de l’alcoolisation fœtale TSAF. (French). A website providing resources and explanation about diagnosing FASD as per Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan.
- The CanFASD Diagnostic App. (English). A point-of-care tool to support clinical decision-making, based on the above algorithm from Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan. Designed for iPad use.
- Two-Eyed Seeing Tools for Screening, Assessment, Intervention and Prevention. (English.) Inspired by Mi’kmaq Elders, Two-Eyed Seeing (TES) tools integrate a traditional healing perspective into the medical assessment process.
Who is part of the diagnostic team?
Across the lifespan of clients, different team members are recommended.
Infants (under 18 months):
- Paediatrician/physician
- Child development specialist with skill set to conduct physical and functional assessments (e.g., speech-language pathologist, physiotherapist, occupational therapist, clinical psychologist)
Preschoolers (18 months to 5 years):
- Paediatrician/physician
- Occupational therapist
- Speech-language pathologist
- Psychologist
School-aged children (6 years to age of majority):
- Paediatrician/physician with expertise in FASD and differential diagnosis
- Occupational therapist
- Speech-language pathologist
- Psychologist
Adults:
- Physician
- Psychologist
- Speech-language pathologist/psychologist with expertise in language assessment
There are also benefits to including others in the clinic team, such as: individuals with living experience (e.g., a peer mentorship program), cultural interpreters, experienced team members who mentor newer ones, social workers, addiction counsellors, justice workers, mental health providers, clinic coordinators, and client supports (e.g., an FASD worker). Working with mothers, families, individuals and caregivers as collaborators in the care process is critically important.
Diagnoses and Designations upon Assessment Completion
There are four possible outcomes following FASD assessment. This section will give an overview of the criteria, but further explanation of each criterion is provided below.
Diagnosis: FASD with sentinel facial features.
Criteria:
- Three sentinel facial features, specific to prenatal alcohol exposure.
- Confirmed or unknown PAE.
- Impairment in three (or more) brain domains (and microcephaly in infants and young children).
Diagnosis: FASD without sentinel facial features.
Criteria:
- Impairment in three (or more) brain domains.
- Confirmed PAE.
Designation: At-risk for neurodevelopmental disorder and FASD, associated with prenatal alcohol exposure.
Note that this is not a diagnosis. This is a designation provided when, for a number of reasons, individuals do not or cannot complete the full diagnostic process. Individuals with this designation must be re-evaluated at an appropriate time.
Criteria:
- Confirmed PAE.
- There is evidence of a neurodevelopmental disorder and a plausible explanation as to why assessment did not provide sufficient evidence of neurodevelopmental impairment OR Individuals who have all three sentinel facial features, but do not have impairment in three (or more) of the neurodevelopmental domains OR true microcephaly in infants and small children.
This designation is never considered when PAE is confirmed absent.
No diagnosis or designation.
Individuals do not meet criteria.
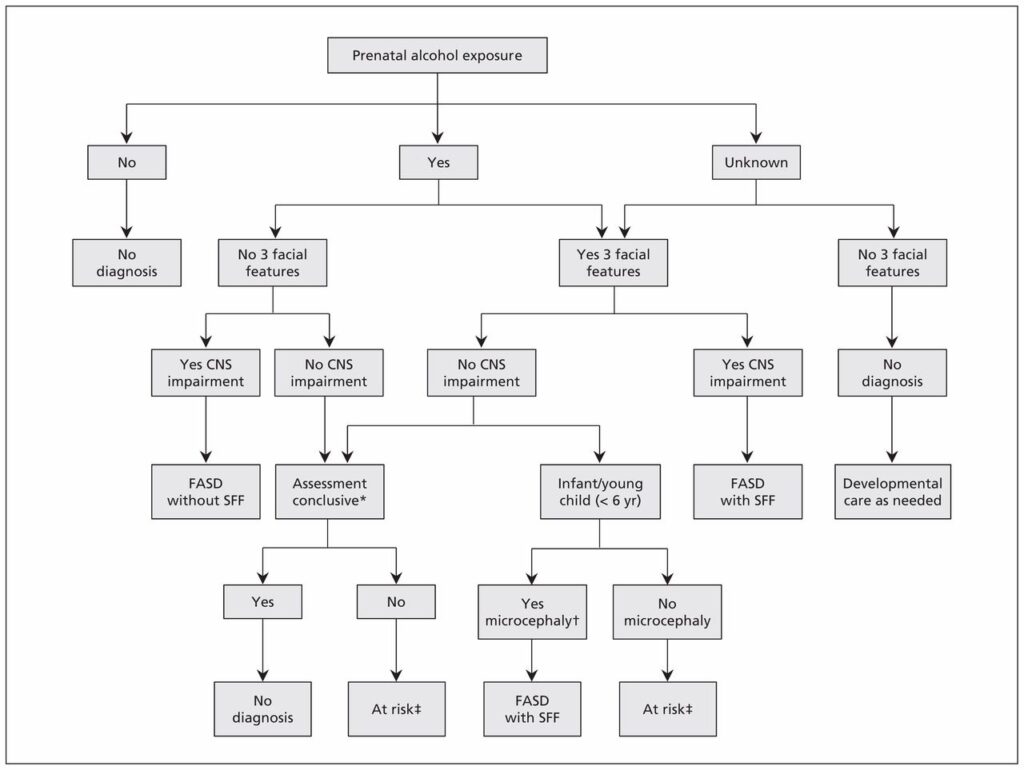
The assessment process can proceed through the following diagnostic algorithm:
The Diagnostic Criteria for FASD
Because of the complexity, a multidisciplinary team works together to provide the FASD assessment.
A diagnosis of FASD includes assessment in three areas: neurodevelopmental brain domains, facial features and confirmation of enough prenatal alcohol exposure to be associated with neurodevelopmental impairment.
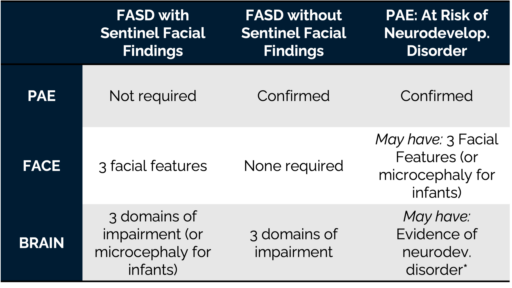
These criteria are summarized in the following table:
* The at-risk designation is considered if an individual has confirmed PAE, and:
- Evidence of neurodev. disorder and plausible explanation for why assessment did not reach 3 or more domains
- 3 facial features without impairment in 3 domains or true microcephaly in infants and small children
Note: Growth, congenital anomalies, co-morbidities, birth defects, sensory, sleep and other pre and postnatal factors all need to be recorded if present.
1. The Neurodevelopmental Assessment
Clients may meet criteria for a diagnosis of FASD if they have significant impairment (-2 standard deviations from the mean) in three (or more) of ten specific neurodevelopmental brain domains:
1. Motor Skills.
Impairment in fine motor skills, gross motor skills, graphomotor skills, or visual-motor integration.
2. Neuroanatomy/Neurophysiology.
Smaller head size, seizure disorder, or other structural brain abnormalities associated with prenatal alcohol exposure (when other etiologies have been excluded).
3. Cognition.
Difficulties with intellectual functioning; i.e., reasoning, problem-solving, planning and/or understanding complex ideas (e.g., the abstract concept of time or money). While Intelligence Quotient (IQ) can be measured in this domain, it has not been found to be an accurate estimate of functional ability due to the wide range of IQ scores individuals with FASD can present.
4. Language.
Difficulties with core language, receptive language, expressive language, or higher-level language skills (e.g., an individual may speak well without fully grasping the content of the discussion).
5. Academic Achievement.
Difficulties with reading, math, and/or written expression, provided the individual has had sufficient and consistent exposure to academic instruction prior to assessment.
6. Memory.
Impairment may be present in overall memory, verbal memory, and/or visual memory; discrepancies may also be present between verbal and nonverbal memory.
7. Attention.
Difficulties in sustaining attention, selectively attending, and resisting distractions.
8. Executive Function, including Impulse Control and Hyperactivity.
Impairment in higher-level skills necessary to meet long-term goals, including working memory, inhibition/impulse control, hyperactivity, planning and problem solving, or shifting and cognitive flexibility.
9. Affect Regulation.
Long-term mood dysregulation (i.e., not a response to life events) that meets DSM-5 criteria for Major Depressive Disorder (with recurrent episodes), Persistent Depressive Disorder, Disruptive Mood Dysregulation Disorder, Separation Anxiety Disorder, Selective Mutism, Social Anxiety Disorder, Panic Disorder, Agoraphobia, or Generalized Anxiety Disorder.
10. Adaptive behaviour, social skills, or social communication.
Impairment in social language, social communication skills or pragmatic language skills, including social vulnerability to manipulation, difficulty understanding personal boundaries, or emotional immaturity.
Resources:
- Appendix F in Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan
2. Measurement of Facial Features
Although typically less than 10% of individuals with FASD have the three sentinel facial features, they are important indicators of PAE and will be affected if exposure occurred during the critical period of fetal development. The sentinel facial features of FASD are:
- Short palpebral fissures (below the 3rd percentile or 2 standard deviations below the mean. Details are available in Appendix 1 of the Canadian guidelines for FASD diagnosis across the lifespan)
- Smooth philtrum (rated 4 or 5 on the 5-point scale of the University of Washington Lip-Philtrum Guides)
- Thin upper lip (rated 4 or 5 on the 5-point scale of the University of Washington Lip-Philtrum Guides)
Note: Infants and young children presenting with all 3 sentinel facial features and microcephaly may receive a formal diagnosis of FASD with Sentinel Facial Features, even if they have yet to meet the criteria for significant neurodevelopment impairment.
Resources:
- FAS DPN Diagnostic Tools: University of Washington software that computes standard deviation values.
- MorpheusQ App: a tool to assist in measurement of facial features, to be used in identification of FASD.
3. Confirmation of Prenatal Alcohol Exposure (PAE)
Effects of PAE have been demonstrated to vary by gender, ethnicity, history, genetics, timing of consumption, frequency and quantity—and it is likely that there are multiple mechanisms through which alcohol impacts fetal development. (For more information, see Appendix 1 (p.14) of Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan.)
There is no safe amount of alcohol during pregnancy.
This means that there is no definitive threshold value for PAE to diagnose FASD. Therefore, there are three possible outcomes when assessing if there is enough prenatal alcohol exposure to be associated with neurodevelopmental impairment:
1. Prenatal alcohol exposure is confirmed present by a reliable source
The diagnostic assessment can continue. A diagnosis of FASD, designation of at-risk, or no diagnosis are all possible results.
2. Prenatal alcohol exposure is confirmed absent by a reliable source
If there has been no PAE, the diagnosis cannot be FASD.
3. Prenatal alcohol exposure is unknown
Individuals can still receive a diagnosis of FASD if PAE is unknown AND if 3 facial features are present.
Information about PAE can be attained through a number of methods. Rajani Clinic Training Services has recently developed A Toolkit to Support PAE Collection in FASD Diagnostic Clinics which may be of use. Other methods may include those listed below.
For these reasons, the diagnostic process should include a complete physical examination, alongside compiling a social and medical history. This includes the dose of alcohol consumed (i.e., the number and types of drinks), as well as the frequency and patterns of drinking.
For other resources and discussion of prenatal alcohol exposure, please see the Identification and Early Intervention tab.
Assessment Report and Recommendations
After assessment and diagnosis are completed, the diagnostic team summarizes the results in a medical report with accompanying recommendations for interventions and support.
The format of the report varies between clinics, but the components should include:
- Why the client was referred to clinic
- Overview of the FASD diagnostic process
- Summary of assessment results:
- Physical exam (including) Facial measurements
- Psychological assessment summary
- Speech/Language/communication assessment summary
- Occupational therapy assessment summary
- Summary of the clients history and current situation, without revealing too much sensitive or private information
- Diagnosis:
- Relevant FASD diagnosis
- Other comorbidities, such as:
- Attentional diagnosis
- Mental health, depression, anxiety, etc.
- Learning disabilities
- Communication disorders
- Adaptive functioning difficulties
- Health concerns
- Identified strengths of the client
- Recommendations should be 10 or less to reduce confusion and increase confidence of the family. These recommendations should be made by the multidisciplinary team together.
Detailed information about how the diagnosis was arrived at should be kept by the clinic in the event that the diagnosis needs to be reviewed in the future. Clinics may also create an additional plain language, simplified report as a summary for clients and families—or creating accompanying letters that families can use for advocacy (e.g., a letter explaining diagnosis and needed supports to the client’s school).
Sample Recommendations:
- Family can link to the local FASD support services to assist with learning about FASD and to follow though on the recommendations
- Share this report with the family doctor, school or support services assisting the client.
- Consult with the family doctor on medications for their relevant needs. They may consult the Medication algorithm for FASD (English | French).
- Begin planning ahead for transition to adulthood and to consider:
- Applying for disability funding
- Building a transition plan
- Explore post secondary options
- Develop life skills
- Consider birth control and sex education
- Update hearing and eye exams annually
Some families experience a “now what?” feeling of helplessness after diagnosis. The goal of the assessment meeting and any follow-ups should be to mitigate this experience. Supportive relationships with service providers should persist prior to, during, and after diagnosis.
During conversation about the assessment results, time should be budgeted for discussion of interventions, supports, and next steps. You may return to your original timeline/pathway, and revisit the questions that have been answered, the ones that may have been missed, and any new ones that have come up. Clinics may also consider having an open door policy for families to return to the clinic if and when they need support.
For more information on services and supports, please visit the Patient and Family-Facing Resources and Services page.
Note on Service Provider Burnout, Compassion Fatigue, and Self-Care
Working with people with FASD, trauma, and other life experiences can be mentally and emotionally challenging. Assessment requires flexibility, patience and care. It has been reported that caregivers of those with FASD (or possible FASD) experience much higher levels of stress and health issues than caregivers of other children with neurodevelopmental disorders.
In addition, when helping others, the benefits of supportive actions can feel far away. Care for FASD is for the long-term; meaningful change can be gradual and incremental, and the true benefits of your support can be difficult to see at any one point in time.
As a clinician, it is important to recognize and acknowledge burnout and compassion fatigue in yourself and the caregivers you are working with.
Meaning and caring burnout and compassion fatigue are forms of physical, emotional and/or mental exhaustion. Strategies to lessen their impact and prioritize self-care will differ from person to person.
Reflect on yourself and how you are being impacted by your work. Can you recognize potential signs of burnout and compassion fatigue?
- Feeling limited motivation, as if you have difficulty finding meaning in your actions or feeling as if you are past the point of caring.
- Feeling overwhelmed
- Feeling isolated or isolating yourself
- Having your personal relationships become affected
- Losing confidence in your work and abilities
- Changes in your feelings of being able to depend on yourself and others
- Changes in your beliefs and worldviews (e.g., questioning your career path)
- Changes in your feelings of safety
Recognizing the signs of burnout and compassion fatigue is a significant step towards addressing your needs. It is important to reflect on the way you are feeling and take intentional steps to prioritize caring for yourself.
Though we all have different needs, consider the following strategies when prioritizing yourself:
Physical Strategies:
Caring for your body through adequate sleep, nutrition, and activity.
Psychological and Emotional Strategies:
Setting boundaries and working with professionals to maintain your mental health. This also includes making self-care one of your priorities.
Spiritual Strategies:
Reorient yourself to the meaning in your life through what speaks to you and feels larger than you, such as journaling, travelling, meditation, community engagement, etc.
Relational Strategies:
Combat isolation through seeking out your relationships; regularly visit friends and those in your community and relate to those around you.
Strategies in Pleasure and Enjoyment:
Invest time in yourself: engage in leisure activities outside of work that bring you satisfaction, gratification, and contentment. This may also include learning new skills and trying new things.
Professional Strategies:
Participate in work activities that increase feelings of satisfaction, effectiveness, and accomplishment, such as professional development or incident debriefing. This can also include working with mentors with experience in FASD and navigating the work-life balance.
Resources for Self-Care
- Lorsque compassion rime avec souffrance. (French.) (2014). A manual that provides definitions, information, and strategies to prevent burnout, vicarious trauma and secondary trauma.
- Skovholt Practitioner Professional Resiliency and Self-Care Inventory. (English.) A self-assessment tool for professionals to explore and understand their burnout and/or compassion fatigue.
Ongoing Learning Resources for FASD Diagnostic Clinic Management
As we learn more about prenatal alcohol exposure and FASD, best practices for assessment, management, and service delivery will grow and change. The best way to stay in the know about current best practices is to connect with other professionals in the field.
There are many events and organizations working hard to educate and update what we know.
Recommended Clinic Team Management Best Practices
- Meet at least annually to discuss concerns, successes, review documents (e.g., the Competency Framework created by Rajani Clinic Training Services)
- Provide training opportunities
- Become involved in research
- Support the clinic coordinator with good training and guidance on clinic process preferences
The Canadian National FASD Database.
CanFASD launched the first comprehensive FASD database in the world, providing key insight into the profile of individuals with FASD.
The database collects real-time data from FASD diagnostic clinics across Canada, helping inform policy and practice at a national level. Information from the database provides data back to each of the diagnostic clinics to help them inform and support their own work.
Diagnostic clinics also are part of the National FASD Database Community of Practice, promoting mentorship and collaboration between clinics across Canada.
Lakeland Centre for FASD, Rajani FASD Diagnostic Clinic Training Services
Lakeland Centre for FASD, Rajani FASD Diagnostic Clinic Training Services provides many educational resources, such as their Competency Framework for FASD Diagnostic Clinics, alongside ongoing training for FASD diagnostic clinics all over Canada tailored to their specific needs.
This clinic has been working since 2002 and has continued to adapt and evolve with new research, best practices, and changes in the field. Rajani FASD Diagnostic Clinic Training Services also hosts an annual meeting for all FASD diagnostic clinics in Alberta.
CanFASD Professional Membership
CanFASD offers several levels of membership, including Individual, Affiliate, and Jurisdictional. Individual membership is split into Professional and Personal Memberships. With a Professional membership, you can stay up-to-date on current research and learning opportunities. Some of your benefits will include:
- Access to the CanFASD Membership Directory: Connect with our 200+ community members, and choose if you would like to join the list!
- Access to member-only events, such as our Research Conversations series
- Real-time project updates to keep you in the loop
- Bi-weekly newsletters with updates and exclusive stories
- Research opportunities to promote your project to our network or find out about projects you can participate in
And much more!
The Biennial Canada FASD Conference
The Canada FASD Conference welcomes researchers, caregivers, individuals with living experience, policymakers, and professionals from across Canada and abroad to share knowledge and perspectives on FASD. This event is hosted in different areas of Canada to give everyone a chance to attend.
To stay in the loop, join the mailing list!
FASD Ontario Network of Expertise (FASD ONE)
If you are in Ontario, you can join the FASD ONE Community of Practice. FASD ONE aims to link people with FASD, caregivers and professionals to services and supports, as well as transferring knowledge and developing resources.
For Additional Learning:
Webinars
Understanding the FASD Diagnosis. (English, auto-generated French subtitles available).
Issue Papers
Papers summarizing key issues related to the diagnosis of FASD include:
Why FASD Diagnostic Assessment is Important (2023)
This issue paper outlines the importance of an FASD diagnostic assessment to supporting and improving outcomes for diagnosed individuals and their families.
Diagnostic Assessment of Preschoolers with Prenatal Alcohol Exposure (2023)
Diagnostic assessment of preschoolers offers an early opportunity to identify young children at risk for behavioural and learning difficulties and provide them with appropriate interventions but identification and assessment at this age can be difficult.
Patient and Family-Facing Resources and Services
Effective management of Fetal Alcohol Spectrum Disorder (FASD) extends beyond diagnosis and requires coordinated, compassionate, and long-term support tailored to each individual’s unique needs. That means consideration of before, during and after diagnosis, including (but not limited to) what can be done while individuals are on the waiting list, how to ease the confusion and fatigue that may come from the emotionally taxing process for individuals and families, and collaborative planning for clear next steps after diagnosis.
This page is meant to guide members of diagnostic teams in delivering coordinated, strengths-based, and lifelong care for individuals with FASD.
It is important to note that for many families, written materials alone are insufficient, especially for families with neurodivergence, limited literacy, or language barriers. At all stages, approaches should be relational, strengths-based, and trauma-informed to prepare families for assessment and sharing diagnostic outcomes.
“Printed documents are just one more thing they have to read. Many of the parents can be neurodivergent themselves, and reading the material does not mean they understand. They need relationships with humans to support them and create that trust.”
Creating a Guide on What to Expect Before, During and After Diagnosis
Many caregivers and individuals can be overwhelmed with the referral and assessment process. They may come into appointments expecting resistance and complications. If on a waiting list, they may worry they have been forgotten about. Given the great amount of information they receive during appointments, they may have difficulties remembering the full detail of everything discussed. The more safeguards that are built in place, the more comfortable the process will be for everyone involved.
Below are some resources that can be offered to help this process. Many resources should duplicate information that is given during conversation and appointments, as different people learn and remember best in different ways.
A comprehensive client and family guide can help standardize care, and answer questions outside of appointments.
In your client and family guide, you could include:
General information about FASD.
Considerations: what diagnosis of FASD can do for you, decreasing the stigma of alcohol use during pregnancy, how to amplify strengths, what PAE info is needed, what is required for diagnosis and encouragement/support of individuals and families in terms of diagnosis and interventions. For example, The ‘I am a Caregiver!’ guide (English | French) provides information and resources about providing care for children and adults with FASD.
Disclosures and consent.
A plain-language explanation of the information that will be utilized, if it will be released elsewhere, and why.
The overall clinic process.
A graphic or timeline can help to demonstrate this information in a different way, such as an infographic (e.g., English). Break down the clinic process, the purpose and information gathered in each appointment, and the after-diagnosis care plans. An expected timeline can help to map out an otherwise confusing process.
- Timeline of clinic process
- List of staff
- Purpose of each appointment
- After-diagnosis care plans
- For younger clients, consider a social story
An appointment schedule.
Provide details of each appointment, including the times, expected durations, addresses, professionals they will be seeing and what the goal of each appointment is.
- Considerations of supports like appointment reminders, transport assistance or help to get online.
“What to Bring” lists.
Different appointments have different expectations, durations and demands. Create a list of documents, records, identification, medications, supports, food, and so on that may be needed at each appointment. Consider splitting lists into “What is Needed” and “What May be Helpful” to promote individuals and families bringing relevant support workers, sensory items, or other beneficial items that will not interfere with assessment or diagnosis. If helpful, you may also include a “What to Avoid” list.
- What is Needed (e.g., documentation, medications, etc.)
- What May be Helpful (e.g., FASD support workers, food for lunch, etc.)
- What to Avoid
“While We Wait” Packet.
Connect individuals with living experience to each other, community supports and provide ideas for activities and strategies while waiting (e.g., community agencies, peer supports, mental health & addiction services, early referral to psychiatry, efforts to determine a comprehensive family history, etc.).
Other resources are available in the Resources for Individuals, Families and Advocates section.
Patient- and Family-Facing Resources for Explaining FASD and Diagnosis
Below are some resources that could be given to clients and families to help explain about the FASD diagnosis.
- A Caregiver’s Guide to Diagnosis. (English | French). This guide is for caregivers for individuals prenatally exposed to alcohol who are going to be assessed for FASD.
- Caregiver’s Guide to FASD Assessment from Piruqatigiit Resource Centre. (English | Inuktitut (ᐃᓄᒃᑎᑐᑦ) | Français). This guide is for caregivers for individuals prenatally exposed to alcohol who are going to be assessed for FASD; this guide is an example of a guide tailored to a specific clinic.
- FASD: A Whole Body Diagnosis. (English, auto-generated French subtitles available). A webinar by Myles Himmelreich who speaks about his lived and living experience, alongside clinical FASD specialists and a parent advocate.
- Frequently Asked Questions – FASD. (English | French). A plain language page to answer questions about FASD, challenge common misconceptions, and discuss prevention, diagnosis, and FASD over the lifespan.
- Discovering FASD Later in Life: Understanding and Embracing a Late Diagnosis. (English, auto-generated French subtitles available). Nancy Lockwood interviews Reinier deSmit about receiving an FASD diagnosis at the age of 56 in this webinar recording.
- How to Explain an FASD Diagnosis to Your Child. (English). A resource for caregivers to help them explain an FASD diagnosis to their child.
- FASD: a guideline for diagnosis across the lifespan. (English | French). 2016. Caregivers and individuals with FASD may benefit from reading the Canadian guidelines for diagnosis, including the Executive Summary and Appendix.
Management and Services After Diagnosis
FASD-specific programs.
Community FASD networks, caregiver support groups, FASD peer support groups, skill-building workshops, counselling services, housing programs, information sessions/lunch and learns, FASD caseworkers, or other supports that are FASD-informed.
Information on funding.
Each province and territory navigates disability funding differently. Funding sources could include those for comorbidities (e.g., ADHD), disability pensions, mental health, or disability services.
Advocacy supports.
Help for caregivers completing paperwork, meeting support services and training/mentorship in FASD advocacy. Supports in talking to schools and employers. Capacity-building programming for caregivers and individuals to help avoid advocacy fatigue.
Intervention supports.
Could include healthcare and allied health considerations, self-regulation strategies, sensory tools, and supports related to age (e.g., school vs. employment, transition into and out of care, etc).
Strength-based solutions.
While providing options for their limitations, what programs or services can be provided to amplify their strengths?
Interventions, programs and supports are the bulk of what many people will be looking for after assessment. Here are some ideas of supports to look for, creating a Next Steps After Diagnosis specific to your area:
Resources on Interventions and Supports
Many resources can be found on the CanFASD page for interventions. Clients can also be referred to their local FASD network (a list can be found on the Referral Pathways page).
- Health Watch Table – FASD | Surrey Place. (English). (2017). A table of recommendations around various health considerations associated with FASD.
- Towards Healthy Outcomes 2.0. (English | French). (2024). The full Towards Healthy Outcomes framework document, including how you can use the framework and implement its core beliefs into your work.
- The “Dreamcatcher” Model of service delivery (English | French). A living document that puts clients, family, community and culture in the centre of services.
Patient- and Family-Facing Resources on Interventions and Supports
Clients and families can be linked to CanFASD pages: Information For Families and Lifespan Intervention. Alongside these pages, below are other resources that could be given to clients and families about interventions and supports for FASD.
- Safety Plan for Families and Caregivers (FASD). (English | French). (2020). A guide on how families with FASD can prepare for difficult situations and what to do in a possible crisis.
- Parenting Indigenous Children with FASD. (English | French). (2021). A guide for caregivers on how to provide the best parenting for the Indigenous child with FASD they care for.
- Organizing FASD Family/Caregiver Support Groups Facilitator’s Guide. (English | French). (2021). A resource to help service providers and FASD caregivers create new or support existing FASD support groups.
Appropriate supports help individuals with FASD life successful and meaningful lives. For many people, diagnosis is the first step towards accessing these types of services: diagnostic clinics play an essential role as a guide for clients and their families towards tailored and relevant support.
Fetal Alcohol Spectrum Disorder Identification, Assessment and Diagnosis Learning Hub
Welcome to the Fetal Alcohol Spectrum Disorder (FASD) Identification, Assessment and Diagnosis Learning Hub! This hub offers flexible, self-directed learning for health and allied health care professionals at all levels of experience, including training, webinars and additional reading to help build core competencies in FASD care.
Training and Online Courses
Online Training for FASD Identification, Assessment and Diagnosis
Multidisciplinary Team Training for Diagnosis of FASD (English | French)
This online FASD curriculum, based on Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan, has been developed to assist professionals in learning the processes and procedures, and in developing the skill set needed to be effective members of a multidisciplinary diagnostic team.
Online Training for Identification of Alcohol and Pregnancy and FASD
Alcohol and Pregnancy | SOGC. (English | French). This online course summarizes current recommendations about alcohol use during pregnancy, and describes best practices for identification, intervention and treatment.
Trauma and Violence Informed Care | SOGC. (English | French). This online course educates about trauma and how to apply the principles of trauma and violence informed care.
Trauma Training Initiative | Alberta Health Services. (English | French). A two-part training program designed to help professionals create safe, compassionate, and responsive environments when working with individuals and families affected by trauma and violence.
FASD and Substance Use Treatment:
- Moving Towards FASD-Informed Care in Substance Use Treatment. (English | French). (2022). Current practices to support individuals with Fetal Alcohol Spectrum Disorder (FASD) who are in treatment for substance use.
- Moving Towards FASD-Informed Care in Substance Use Treatment: Version 2 Adults and Youth (English | French). (2024). An expansion of the previous guide with updated information about FASD-informed practice and an added focus on developmental considerations for youth with FASD.
Online Training for Management, Supports and Interventions for FASD
Mental Health Resource and Practice Guide. (English). A toolkit for frontline mental health counsellors/therapists, prevention mentors, crisis workers, community mental health providers and those who work directly with individuals with FASD.
Towards Healthy Outcomes 2.0. (English | French). (2024). The full Towards Healthy Outcomes framework document, including how you can use the framework and implement its core beliefs into your work.
Other training is available within CanFASD Online Courses.
Fundamentals of Identification and Diagnosis.
Fetal alcohol spectrum disorder: a guideline for diagnosis across the lifespan. (English | French). These guidelines are meant to help assist multidisciplinary teams through this complex diagnosis, leading to improved health services and creating a positive impact on the health and well-being of children and adults with FASD across their lifespan. Executive Summary | Appendix 1.
Further Learning on Diagnosis and Diagnostic Clinic Structure
- FASD Assessment & Diagnostic Clinic Waitlist Toolkit. (English). Available upon request from Rajani Diagnostic Clinic Training Services. A toolkit designed to aid clinics in creating and navigating their waitlists.
- A Competency Framework for FASD Assessment and Diagnostic Clinics. (English). Available upon request from Rajani Diagnostic Clinic Training Services. A framework to offer guidance to clinicians and team members, allowing clinics to measure strengths and areas for improvement to excel in assessment and diagnosis.
- Understanding FASD Diagnosis. (English, auto-generated French subtitles available). 2022. A webinar exploring what diagnosis looks like in Canada, including clinic models, team members, and walking through the assessment process.
Learning on Stigma and Communication
Common Messages: Guidelines for talking and writing about FASD. (English | French). Updated annually, the purpose of this document is to encourage consistency in how we talk about FASD and the issues related. It outlines key statistics, emerging research, how to frame topics, and best practices related to language use.
Language Guide. (English | French). This guide gives alternative words or phrases to talk about FASD in an effort to promote the dignity of those living with FASD and their families.
Mental Health Structural Stigma in Healthcare Course (English | French). A course intended to help identify and understand structural stigma in their organizations.
Learning on Breastfeeding
Drinking Alcohol while Breastfeeding: Guidelines for Consultants. (English | French). (2016). A desk reference on how to reduce the negative effects of alcohol while supporting breastfeeding. Includes a table on time alcohol takes to clear breastmilk as per mother’s weight.
CanFASD Issue Paper: Alcohol and Breastfeeding. (English). A CanFASD issue paper summarizing what is known about alcohol and breastfeeding, including lactation and child health.